‘Breast Cancer Unawareness’: The Debate Over Dense Breast Notification Legislation (Updated)
Beyond the mainstream breast cancer awareness movement, with its pink billboards and merchandise, a lower-profile campaign focused on raising awareness about breast density has been building steadily.
UPDATE, November 4, 8:53 a.m.: Pennsylvania Gov. Corbett signed the Breast Density Notification Act into law Friday. “I am proud to sign this bill today to improve breast cancer detection and ensure our daughters, our mothers, our wives, our sisters and our friends have earlier access to lifesaving care,” he said.
The new law will go into effect in 90 days.
The bright pink breast cancer awareness campaigns advertised on buildings, television screens, and magazines every October guarantees almost all Americans are “aware” of the disease that kills some 40,000 women in the country every year. But beyond the mainstream breast cancer awareness movement, a lower-profile campaign focused on raising awareness about breast density has been building steadily.
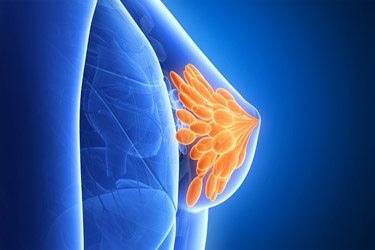
Breast density measures the ratio of fibrous, glandular, and fatty tissue on a four-part scale called BI-RADS. A breast with more fibrous and glandular tissue and less fat is considered dense. Experts say it’s more difficult for a mammogram to spot a tumor behind glandular and fibrous tissue; it’s easier for the machine to see through fatty tissue.
Although breast density has been indicated on the report from the radiologist to the physician since the early 1990s, it has traditionally been left up to the doctor reading the report to share the information—or not—with his or her patient, depending on how they interpreted the report’s significance when considered along with other breast cancer risk factors.
Instead of tinting fountain water or brokering branding deals, as has been the case with many breast cancer awareness efforts, breast density awareness advocates are out to change that protocol through legislation. The first such bill was passed in Connecticut in 2009. Since then, at least 19 breast density notification bills have been introduced in state legislatures around the country, and 13 have passed into law.
Pennsylvania is poised to be next. When passed, the Breast Density Screening Notification and Screening Insurance Coverage bill will require that women be directly notified of their breast density, along with a generic explanation explaining breast density. The bill recently passed both chambers of the state legislature and is headed to the desk of Gov. Tom Corbett.
Here’s the full text of the notification that will be included on mammogram reports:
This notice contains the results of your recent mammogram, including information about breast density. If your mammogram shows that your breast tissue is dense, you should know that dense breast tissue is a common finding and is not abnormal. Statistics show as many as 70% of women could have dense or highly dense breasts. Dense breast tissue can make it harder to find cancer on a mammogram and may be associated with an increased risk of cancer. This information about the result of your mammogram is given to you to raise your awareness and to inform your conversations with your physician. Together, you can decide which screening options are right for you, based on your mammogram results, individual risk factors or physical examination. A report of your results was sent to your physician.
A department of health spokesperson told Rewire Gov. Corbett is expected to sign the bill.
A companion bill has been sitting in committee since January; it would require health insurance providers to cover doctor-recommended supplemental screenings such as MRIs and ultrasounds “if a mammogram demonstrates heterogeneous or dense breast tissue based on the Breast Imaging Reporting and Data system established by the American College of Radiology or if a woman is believed to be at increased risk for breast cancer due to family history or prior personal history of breast cancer, positive genetic testing or other indications.”
Origin of the Breast Density Awareness Movement
In 2003, Nancy Cappello received her 11th annual clean and clear mammogram.
Two months later, during a routine gynecological exam, her doctor felt something in her breast and advised a follow-up ultrasound. Cappello told Rewire that she wasn’t particularly worried about the lump because she had had years of clean mammograms, and she had no history of first-degree relatives with breast cancer in her family and every reason to believe she was healthy.
Then everything changed.
“I’m lying on by my back, and all of a sudden they have six people descending on me,” said Cappello. “They saw something suspicious. It was illuminated, clear, on the ultrasound.”
A biopsy revealed she had stage-three breast cancer that had metastasized to 13 lymph nodes.
Bewildered, she asked her doctors how her cancer could have been missed, despite following recommended protocols. “Well, Nancy, it’s very hard to find a cancer with dense breasts,” she was told.
“I said, ‘Shouldn’t I know this?’ And he said, ‘Well, we don’t tell you.’”
Cappello calls this knowledge gap “breast cancer unawareness.”
“You can read a lot of stuff about breast cancer, and I will tell you the majority of the stuff you’re reading doesn’t mention breast density, and it is the number one predictor of cancer missed by mammogram,” said Cappello. After six surgeries, a year and a half of aggressive treatment, and some research, Cappello launched an effort to mandate that mammograms include breast cancer density information in her home state of Connecticut.
Controversy Over the Bill
Cappello frames her efforts as a straight-forward issue of informed consent. But not all stakeholders in the professional breast cancer community agree with Cappello that including a breast density report on the patient’s mammogram report is a good thing.
For the most part, it’s professional medical communities that have expressed concern about the trend, which makes sense given that professional medical associations generally don’t approve of legislation that reaches into examination rooms.
Though Cappello and other breast density awareness activists say the American College of Radiology (ACR) and the American Congress of Obstetricians and Gynecologists (ACOG) are against the bill, representatives for both organizations, when speaking with Rewire, were careful to specify that they are neutral regarding direct-patient notification. They both presented their concerns as wanting to make sure “everyone was on the same page” regarding possible unintended consequences of changing the protocol.
In Pennsylvania, ACOG hired lobbyists to help shape the language of the bill.
Dr. Kurt Barnhart is chair of the Pennsylvania chapter of ACOG. He says he and his organization worked with legislators to change the original language of the notification so it wouldn’t “alarm people.”
“We still don’t particularly like the idea that legislators are telling us how to practice medicine,” said Barnhart. “But we weren’t going to get in the way of a well-intended bill, as long as we felt the ramifications of a well-intended notification could be managed properly.”
Barnhart says the group doesn’t yet know the extent of the bill’s possible unintended consequences, but the notification will of course generate follow-up calls to the office, more consultations, and more follow-up MRIs and ultrasounds.
In a conversation with Rewire, Shawn Farley, an ACR spokesperson, echoed these concerns. The ACR issued a formal statement on notification bills that put it this way:
It is well known that greater breast density results in lower sensitivity for mammography. … While the ACR supports and promotes the practice of patient education and encourages Americans to take charge of their own care, it is less clear how patients may interpret the same information if included in a patient summary. While the ACR is not opposed to including breast parenchymal information in the lay summary [given directly to the patient], we urge strong consideration of the benefits, possible harms and unintended consequences of doing so.
The ACR statement explains that because breast density is somewhat subjective, multiple conflicting reports may manufacture a lack of trust in mammography for general patients. They are concerned that notification will instill a false sense of security in women with fatty breasts. They also state that the “significance of breast density as a risk factor for breast cancer is highly controversial,” and “there is no consensus that density per se confers sufficient risk to warrant supplemental screening.”
While ultrasound and MRI tests are more sensitive, they also produce false positives.
“The last two major scientific studies that have been done have both shown that they result in more false positives than mammography does,” said Farley. “Since breast ultrasound and MRI do result in more false positives than mammography, you may have additional and ultimately unnecessary workups and testing being done. This could include breast biopsies.”
ACR has created a website to provide information for primary care physicians and OB-GYNs during follow-up conversations regarding breast density and breast cancer risk.
Another concern is that unnecessary screening may not always be covered by insurance, creating unnecessary anxiety and financial hardship. Cappello dismisses the anxiety argument. “All the concern of the profession does not solve the fact that dense tissue impacts the accuracy of a women’s mammogram, and shouldn’t she know it?” she said. “I would trade in my advanced stage cancer for an early cancer any day.”
Not everyone feels the same way. Kelly, 50, is a Pennsylvania resident currently being treated for breast cancer. (She chose not to be identified by her real name because some family members don’t know about her condition.) Kelly has dense breasts, and was diagnosed with stage-two cancer earlier this year. She says she falls on the side of the professional organizations.
“I don’t wish this on anyone but … I feel like for me, all [being notified of dense breasts] would have caused me was worry. My oncologist said at one point, we would love to tell you that we know why people get breast cancer, and it’s occasionally a genetic component, but she said if that were the case than everyone who had those same conditions would have cancer,” she said. “We don’t know what that other factor is or whether it’s one factor, or other factors, because not everyone with dense breasts get breast cancer.”
Advocates plan to reintroduce a federal bill soon.
