On Maternal Mortality, Why Africa Falls So Far Behind
What leads the women of Africa to their graves during pregnancy and childbirth? Nutrition, education, high fertility, female genital mutilation, improper care at delivery and inadequate health facilities all play a part.
A very distraught old woman came to Edna Adan Maternity Hospital in
Hargeisa, Somaliland, appealing to us to help her transport to the
hospital a woman who had given birth five days earlier and who still
had the placenta inside her. Those of us at the hospital are not sure
how this could be possible and we ask her again whether she means five
hours. She is sure about the number of days, and quotes the day the
woman had delivered which, indeed, was five days earlier. She also
tells us that the woman may not be alive by the time we get to her.
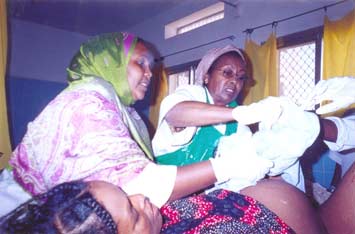 Safe Motherhood Project At WorkWe prepared the ambulance, put in our emergency obstetric kit and
Safe Motherhood Project At WorkWe prepared the ambulance, put in our emergency obstetric kit and
set out towards the home at the opposite end of town from our hospital.
We come to a hut with quite a few neighbors and onlookers standing
around.
Before we get to the patient, we could have been guided to the woman
by the smell coming from inside the hut. We find a woman who has bled
for several days, is very infected, febrile, dehydrated, has no
recordable blood pressure and a weak, rapid pulse. We cannot understand
how she could have survived this long in this condition. Answers to our
questions would come later, but right now, we needed to get an IV line
going, and once in, we put her in the ambulance and headed for the
hospital where blood transfusions and medical care would be ready for
her. We also brought along the baby.
Once she picked up, we got the placenta out, started her on high
doses of antibiotics and the woman miraculously recovered and went home
a week later.
Our burning question was why did they
wait for five days before they looked for help when the placenta
refused to come out after the baby was born?
The unfortunate answers were: (1) We thought we would wait and hoped
that it would come out later. (2) When it took too long to come out,
her husband suggested that they try Somali Traditional methods to get
the placenta out. (3) When this failed, they tried spiritual chants and
prayers. (4) By the third day, they feared that if they report this to
the hospitals, the old woman who had attended the delivery would be
denounced to the government. (5) Finally, the woman became so ill that
they feared they would not be able to afford the cost of the medicines
she would need to treat her.
 Edna Adan Maternity Hospital in Somaliland
Edna Adan Maternity Hospital in Somaliland
Luckily, they got the
courage to come to us and we were able to treat her free of charge,
although we had our conditions for this free treatment: the woman who
had attended the delivery would have to agree to spend five days at our hospital
to be shown how to conduct a normal delivery and to know which
conditions to refer immediately. To this, she agreed, and hopefully,
this situation never will be repeated.
This was just
one example of what practicing midwifery in our part of the world
entails. My theory is that women in Somaliland die because of ignorance
on their part and on the part of those assisting them. Poverty is a
strong factor that prevents women from seeking help because they
convince themselves that they cannot afford the cost of modern medicine
and would rather consult the local traditional healer who often causes
more complications.
Pregnancy, Childbirth Still Killing Women
In
1945, diplomats representing the countries of the world at the end of
the Second World War gathered in New York and proposed the formation of
a global health organization. In April 1948, the constitution of the World Health Organization was passed, with its first article stating, "Health is a fundamental Human Right."
Sixty years later, that noble declaration seems to have had little
effect on the maternal mortality rate of women in the developing
countries. The women continue to die of causes that have been
eliminated in countries where efficient, safe and adequate health care
have been made available for their women.
As far as African
women are concerned, we seem to have very few rights, particularly in
the area of safe reproductive health care. We fare the worst compared
to women in other continents. In my 48-year experience as a midwife, I
see very little improvement in the conditions under which our women
progress through their pregnancies and childbirth. It’s a situation
that shocks me even more today when I witness the advances that have
been made in medical care elsewhere during the past half-century.
Why Africa Falls Behind
What
leads the women of our continent to their graves during pregnancy and
childbirth? As I describe below, the reasons fall into six categories:
nutrition, education, high fertility, female genital mutilation,
improper care at delivery and inadequate health facilities.
Nutrition:
Sub-Saharan countries are affected by increasing degradation of the
environment — which we commonly call desertification — due to
frequent droughts, cutting down of trees, soil erosion and poverty.
Superimposed on this are frequent wars and instability that cause
displacement of peoples and which negatively affects the nutritional
status of those living off the land.
While little girls are
the mothers of tomorrow, we all know that they are fed the leftovers
from whatever the family is eating. If lucky, she occasionally gets a
bone to nibble at. During her childhood, who thinks about the growth of
the bones of these little girls? Does anyone worry that her growth may
become stunted because of chronic malnutrition and anemia? That she
might develop a contracted pelvis? What will happen when she gets
married and her narrow pelvis cannot permit the passage of the babies
she will be expected to bear and produce? How many women have access to
a health facility that can perform a Caesarean section to save the
lives of the baby and its mother before the labor becomes obstructed?
Education:
Quite often, when a family has to decide which of their children can be
sent to school, it is often the girls who are left behind. We find that
illiteracy affects the health and survival outcome of women. The lower
their education level, the higher their risk of health problems,
including those associated with their reproductive life.
An
illiterate woman is not able to seek her rights because she is not even
aware that she has any rights at all. She considers herself "owned;"
first by her family, then by her husband and later by his sons.
High Fertility:
Once the girl is married, immediate and frequent fertility is expected
of her without taking into consideration whether or not her body can
take care of the baby she will conceive. Our women, therefore, produce
as many children as they can to ensure their place in their new home.
In my work, I often witness women having baby number 9 or 10, and also
some having baby number 12, 13, 14, 15 or 16 and, once, baby number 21!
FGM:
As if all her other misfortunes were not enough in themselves, harmful
traditional practices such as female genital mutilation (FGM) are
performed on them and affect the health of women and children in many
African countries, including mine. FGM affects and damages the perineum
and the pelvic floor muscles of women and is a major cause of
laceration of the perineum during childbirth, as well as damage to the
urethra and rectum resulting in fistula formation.
This is
among the most tragic situations and has shocked me so much that I
became the first Somali woman to publicly cry out against FGM in 1976,
well before those who would like us to believe that they are fighting
against a new enemy that they have discovered. Thirty years later, even
though umpteen campaigns have been held and many have joined the
struggle, millions of little girls continue to be cut, mutilated and
affected.
To show the extent of the problem, I developed a
study at the Edna Adan Maternity Hospital on the status of women who
come to our clinic and FGM. Regretfully, and contrary to anecdotal
reports stating that there has been a decline in the practice, we
discovered that 97 percent of the women attending our prenatal clinic
have some form of FGM, and 98 percent of them have the most severe form
of it. I am still working on the final results of this report, but it
is clear that there has to be an FGM strategy that is different and
more effective than that which has been used in the past.
Time of Delivery: Women having babies who
are at a time of their greatest need for skilled medical or midwifery
assistance are often at the mercy of relatives or other individuals who
have received no or insufficient training in the care of women during
childbirth. The woman does not know nor seek proper medical care
because she does not know that this is her right. Many women die of
obstetrical mismanagement with her relatives blaming her misfortune on
"evil spirits" or "the evil eye of other women who were jealous of her
baby."
Health Facilities: The health
facilities are so ill-equipped and poorly staffed that even if women
get taken there, there is very little that can be done for them. More
often than not, women arrive at these health facilities when their
situation is too advanced and cannot be helped. How can infections be
avoided when many health facilities have no water, gloves,
disinfectants, sterilizers or dressings?
Charting a Better Path
Delegating
women to a second-class status does not necessarily raise men to a
first-class status. When when they do, they are denying their sisters,
wives and daughters the education, decision-making and the possibility
to rise to their fullest potential. In short, men lose when they
prevent women from becoming full partners in all the challenges that
life brings.
The prevention of maternal mortality is the
basic right of all women and must be made a priority in all developing
countries. The urgency of the situation warrants vastly heightened
attention. Otherwise, the pledges and statements of health as a human
right will continue to be words printed on paper made from the wood of
the trees that have been cut down — and thus only contributing to more
degradation of the environment, poverty and misery.
This article was first published by On The Issues magazine.
